After an eye has been removed surgically, a socket remains. This is the space between the back surface of the eyelids and the conjunctiva.
Over time the ocular prosthesis can cause tissues to stretch and scar. This in turn may make the ocular prosthesis unstable causing it to easily fall out, or making it difficult to put in. Eye socket surgery aims to create a socket that will comfortably hold an ocular prosthesis.
What is post enucleation socket syndrome?
After eye removal surgery a socket is created into which an ocular prosthesis may be fitted. Problems may arise if over time the socket becomes smaller due to scarring. This may cause the ocular prosthesis to become unstable and fall out. Over time the lower eyelid may become stretched and lax due to the weight of the prosthesis, further adding to instability of the prosthesis. Equally if the socket is too large the ocular prosthesis can move around in the socket and cause increased discharge. A large socket is often due to either no orbital implant or too small an implant. In addition the low volume of tissue in the orbit leads to a superior eyelid sulcus or sunken appearance. The upper lid may droop, which is also know as eyelid ptosis.
Top - a diagram of an orbit after eye removal surgery (enucleation) and the placement of an orbital implant in order to create a shallow eye socket in which an ocular prosthesis may be worn; Bottom - A diagram showing an orbit after eye removal surgery without an implant: the socket is deep meaning the ocular prosthesis will also be larger and heavier leading to post enucleation socket syndrome
What surgical procedures are performed in socket surgery?
The surgical procedure performed will depend upon the problem in the socket. Often more than one procedure is carried out.
Lateral tarsal strip
To correct lower eyelid laxity a lateral tarsal strip may be performed. A small incision is made at the outer angle of the eyelids within a natural skin crease. The eyelid is tightened by shortening it (removing a small piece of it) and then reattaching it to the bone at the side of the eye. The operation should take 30 - 45 minutes to complete and is usually carried out as a day case. Most operations are carried out under local anaesthetic without sedation. After anaesthetic drops have been put in both eyes, an injection of local anaesthetic is given just beneath the skin of the lower eyelid. This is similar to dental anaesthesia and usually takes less than 30 seconds to give. The sutures used are dissolvable.
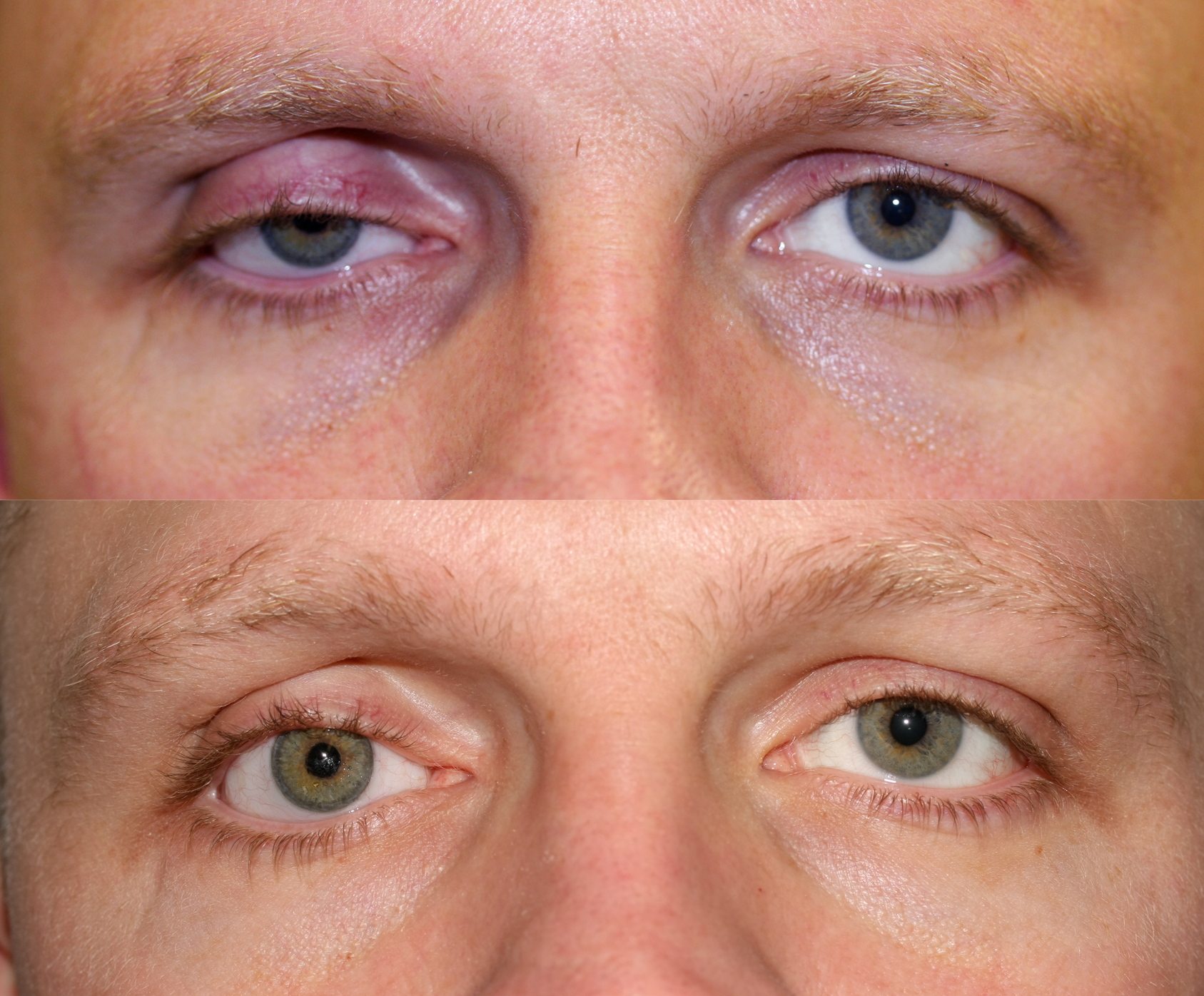
Top - right ocular prosthesis associated with upper eyelid ptosis; Bottom - right upper eyelid ptosis surgery has been performed
Mucous membrane graft
The socket is lined naturally with conjunctiva. In some eye sockets the conjunctiva shrinks and extra socket lining needs to be added. The best socket lining is the wet skin on the inside of the lip, also known as mucous membrane. Usually an area approximately 1x2cm is taken. After the graft has been taken the inside of the lip heals up over the next 1-2 weeks. The graft is sutured into the socket. Frequently, fornix deepening sutures are also placed (see below). This procedure is usually carried out under general anaesthesia.
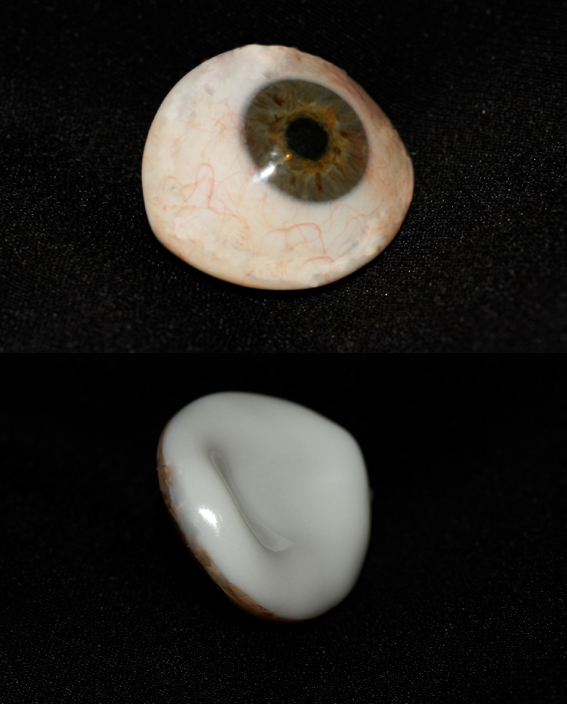
An ocular prosthesis. This is hand fitted and moulded to fit in the eye socket
Fornix deepening sutures
The fornix is the cul de sac or space behind the eyelids. It is into this space that the ocular prosthesis sits. Fornix deepening sutures are placed to enlarge this space or to maintain it after mucous membrane graft surgery to the socket. A permanent suture is passed through small rubber tubing on both the inside and outside of the eyelid. This rubber tubing stops the suture from cheese-wiring through the eyelid. The suture also passes through the bony orbital rim beneath the eyelid to anchor it below. The fornix deepening suture is removed at 6 weeks in clinic.
Secondary orbital implants, orbital implant exchange and dermis fat grafting
One of the main causes of post enucleation socket syndrome is a lack of orbital tissue volume, which in turn creates a socket space that is too large. Surgery can be carried out to increase the volume of tissue in the orbit. This is achieved by placing an orbital implant or dermis fat graft. These days, at the time of eye removal surgery an orbital implant is usually placed - sometimes an orbital implant is not placed due to severe infection or extensive trauma. Some people had implants placed many years ago that are now too small. Some people have had eye removal surgery many years ago before orbital implants were routinely used and therefore don’t have an orbital implant. If an implant is already in place and needs to be larger an orbital implant exchange may be carried out. The old implant is removed and a larger one replaced. The new implant may be of the same material or a new type. If there is no implant in place, one may be inserted surgically. If an old implant is extruding and exposed it may have to be removed. A dermis fat graft may be placed instead of a secondary implant in this situation. A dermis fat graft is taken from the side of the abdomen (tummy) or the buttock. It consists of skin with the top layer of skin removed and a ball of fat attached to it underneath. The dermis fat graft takes the place of the orbital implant and the eye muscles are sutured to it. If an implant extrudes an alternative to removal and replacement is burring and patch grafting. This can only be done if the implant is hydroxyapatite. The exposed implant is drilled down and a graft of tissue (temporalis fascia = tissue around the temple muscle) placed over the burred down implant. The conjunctiva is then sutured in front of the graft.
What are the benefits of eye socket surgery?
Surgery should create a socket that can comfortably hold an ocular prosthesis. Surgery may improve the movement and stability of a prosthesis. A shallower socket and therefore smaller prosthesis will result in less discharge from the socket. Surgery that increases the volume of orbital tissue by secondary implant or dermis fat graft may reduce the amount of upper eyelid sulcus.
What are the alternatives to surgery?
In some situations an ocularist may be able to reshape the ocular prosthesis so that it fits better in the socket. Sometimes simply polishing a prosthesis can reduce the amount of discharge from an eye socket.
What will happen if I decide not to have surgery?
If the socket is shrinking making it difficult to retain a prosthesis, eventually you may not be able to fit a prosthesis in the socket. If the prosthesis has become unstable it may continue to fall out or do so more easily.
What will happen before surgery?
Before the operation you will attend a consultation with Mr. McCormick. He will listen to your problems, examine your eye socket and explain treatment options including risks and benefits. He will also ask about other medical problems you have, medications you take (bring a list or the tablets themselves with you) and any allergies. You will be asked to read and sign a consent form after having the opportunity to ask any questions. You may also see a preoperative assessment nurse. He/She will carry out blood tests and an ECG (heart tracing) if required. They will also advise you if you need to starve before the operation.
What should I do about my medication?
In some cases you may be asked to stop or reduce the dose of blood thinning tablets like: warfarin, aspirin, clopidogrel (plavix), dipyridamole (persantin), ticagrelor, apixaban, dalteparin, rivaroxaban. This decision is made on an individual basis and you should only do so if it is safe and you have been instructed by your GP, surgeon or anaesthetist. This will be discussed with you before surgery. Other medication should be taken as usual. You should avoid herbal remedies for 2 weeks prior to surgery as some of these may cause increased bleeding at the time of surgery. You should avoid non steroidal anti inflammatory medications for 2 weeks prior to surgery. Other medication should be taken as usual.
What are the risks and possible complications of surger?
All surgery caries a risk of bleeding and infection, both are fortunately uncommon in these operations. Infection might present as increased swelling and redness of the skin. There might also be yellow discharge from any wounds or the socket. It is treated with antibiotics. Bleeding may present as fresh blood oozing from the site of surgery or a lump appearing near the wound after the operation. Simple pressure on a skin wound is usually enough to control minor bleeding. Whenever the skin is incised a scar may form. Every attempt is made by the surgeon to minimise and hide scars but sometimes they can be visible. Orbital implants have a small risk of extrusion. This means that at some time after surgery the tissue covering the implant is lost and the surface of the implsnt is exposed. This can lead to infection. It usually means surgery to cover the implant or to remove it. You should have the opportunity to discuss the risks of anaesthesia with your surgeon or anaesthetist prior to surgery. Three types of anaesthesia are used for these procedures: local anaesthetic, local anaesthetic with intravenous sedation and general anaesthesia. Sedation means that you are breathing for yourself and don’t have a breathing tube inserted but you are very relaxed and sleepy and often don’t remember the operation. General means you are completely asleep with a breathing tube inserted.
What should I expect after surgery?
After surgery you may experience pain. Simple paracetamol is usually enough to control this. If not cocodamol (paracetamol + codeine) may be used instead but not as well as. A non steroidal anti inflammatory drug such as ibuprofen may also be used. The eyelids may be swollen and bruised. The swelling usually gets worse gradually over the first 48 hours and then improves over 2 weeks. For the first 2 weeks the eyelids may be sutured together. This tarsorrhaphy suture is removed in clinic at your 2 week review. Unless you have had minor lid surgery you should not wear your ocular prosthesis for 10 weeks following surgery. In its place a clear plastic conformer will have been inserted at the time of surgery. This is to allow the socket swelling to settle after surgery. This is the same type of conformer that will have been placed at the time of your original eye removal surgery. Mr. McCormick will refer you to an ocularist who will see you 8-10 weeks after surgery. He/She will refit your ocular prosthesis or create a completely new one. You may also see the ocularist in the intervening period to clean the conformer.
Post-operative instructions
The need for pain control medication is very variable. For many simple paracetamol or cocodamol are adequate. Ibuprofen or other non steroidal tablets may be added if required. Always read the label before taking medications. If an eye pad is placed it should remain until the next morning when you may remove it. For the first 10 days clean the eyelids and any skin wounds using either sterile water sachets or boiled water that has cooled down and sterile cotton wool balls. Apply Chloramphenicol ointment to the eyelids and any wounds, four times a day for 2 weeks. Follow up appointment 2 weeks later for eyelid suture removal. For cleaning instructions for the conformer and artificial eye please click here - www.robinbrammar.co.uk.